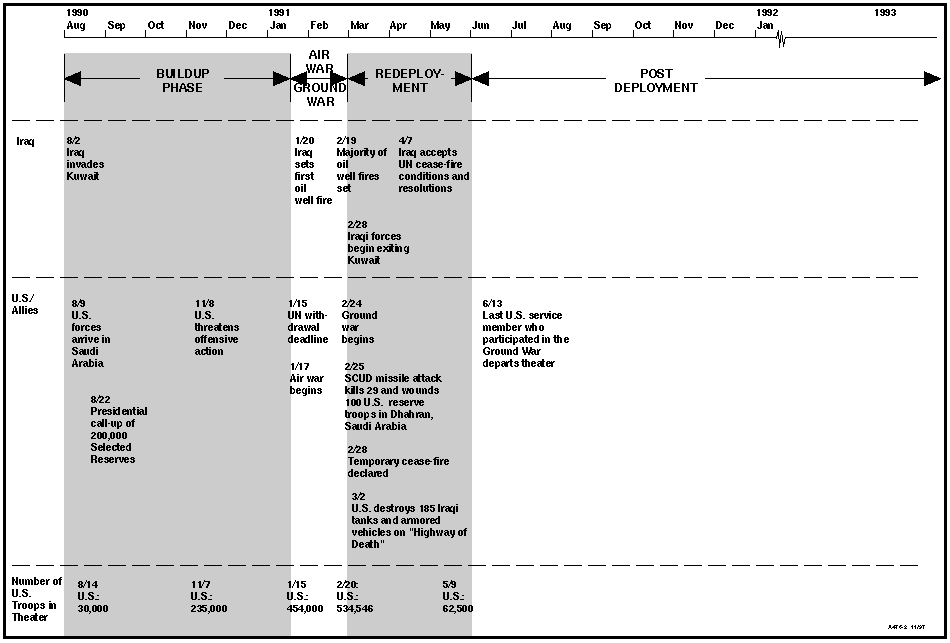
Figure 1.1--Operation Desert Storm/Operation Desert Shield Timeline
Between August 1990 and June 1991, the United States deployed approximately 697,000 military personnel to the Persian Gulf in Operations Desert Shield and Desert Storm (Presidential Advisory Committee, 1996). Over nearly a six-month period, mobilization of U.S. forces to the Persian Gulf proceeded at a pace unprecedented in military history (Ursano and Norwood, 1996). By August 14, 1990, approximately 5000 troops of the 2nd Brigade, 82nd Airborne Division were in the Gulf region (Martin et al., 1996). Less than a month later, approximately 150,000 service personnel were in the Gulf theater. By year-end 1990, a total force exceeding 372,000 troops had been deployed (Spektor, 1998), with this number rising to approximately 535,000 by March 1991 (Holsenbeck, 1996).
Military personnel of both genders, numerous racial/ethnic groups, and ages from 17 through 65 years were deployed. Of the total troops deployed, 84 percent were active-duty personnel and 16 percent were in a reserve or guard component.
Initial deployment of U.S. forces had been intended primarily as a show of force, with the expectation that Iraq would exit Kuwait once confronted by the presence of U.S. troops and the weight of world opinion (Martin and Fagan, 1997). By late October, however, Secretary Cheney announced that Coalition forces would take offensive action to force Iraq out of Kuwait, thereby ending any expectation of an early end to the campaign (Wright, Marlowe, and Gifford, 1991).
In late November, the U.N. Security Council imposed a deadline of January 15, 1991, for Iraqi withdrawal from Kuwait, sanctioning the use of force against Iraq (Gifford et al., 1996). Upon Iraq's failure to withdraw, Operation Desert Storm was initiated on January 17. Beginning with a series of intensive air attacks, Operation Desert Storm culminated in a massive, but brief, ground offensive by Coalition forces. On February 28, four days after the ground war had begun, a temporary cease-fire went into effect. As Iraqi forces began withdrawal from Kuwait, however, sporadic attacks on U.S. forces continued. On March 2, 1990, in the last major battle of the war, U.S. forces engaged a retreating Iraqi column that had charged across the front of the 1st Brigade, 24th Mechanized Infantry Division (Martin et al., p. xxix, 1996). The result was the destruction of the fleeing Iraqi soldiers and of every Iraqi vehicle, including 185 tanks and armored vehicles, 400 trucks, and 34 artillery pieces. The location of this battle became known as the "Highway of Death." As peace was restored, U.S. forces withdrew from the Persian Gulf even more rapidly than they had been initially deployed. By June 13, only two months after formal end to hostilities, the last U.S. service members who had participated in the ground war itself had left the region, replaced by peacekeeping forces. (A timeline depicting key events of Operations Desert Shield and Desert Storm is shown in Figure 1.1.)

Figure 1.1--Operation Desert Storm/Operation Desert Shield Timeline
Table 1.1 shows the wide array of symptoms that have been reported by Gulf War veterans in both clinical programs. They range from potentially minor, frequently self-limiting conditions (e.g., headache) to more serious conditions. The most common symptoms can be associated with multiple conditions (e.g., sleep problems are symptomatic of sleep apnea, fibromyalgia, depression, and other medical conditions), and frequently lack a clear-cut organic explanation. They may be attributed to either physiological or psychological conditions, or to a combination of both. Psychiatric and physical illnesses are not mutually exclusive and frequently coexist (Engel and Katon, 1996).
Table 1.2 shows the most common diagnoses assigned to veterans in the CCEP and VA Registry. The most common categories are musculoskeletal diseases; symptoms, signs, and ill-defined medical conditions (SSID); and psychological disorders. Diagnoses within the musculoskeletal area include rheumatoid arthritis, degenerative disorders, fibromyalgia, tendonitis, pain in joint, bursitis and lower back pain. Many of these are wear and tear disorders that could be expected in physically active military populations. Diagnoses within psychological conditions include somatoform problems (e.g., tension headache), mild or stress-related anxiety, depression, and posttraumatic stress disorder. The symptoms, signs, and ill-defined conditions (classified according to International Classification of Diseases, ICD-9, Codes) include "symptoms, signs, abnormal results of laboratory or other investigative procedures and ill-defined conditions regarding which no diagnosis classifiable elsewhere is recorded."[2] The most frequent symptoms in this category (e.g., fatigue, headaches, sleep disturbance, memory impairment, and digestive complaints) are virtually identical to those reported by the group of veterans as a whole in Table 1.1 (Joseph, 1997).
Ten Most Common Symptoms Reported by Program Participants
(Percent)
| CCEP (N=18,075) | VA Registry (N=52,216) | |||
| Reported Symptom | Chief (percent) | Any of top seven (percent) | Any of top three (percent) | |
| Asymptomatic | 10 | 10 | 12 | |
| Joint pain | 11 | >49 | 17 | |
| Fatigue | 10 | 47 | 20 | |
| Headache | 7 | 39 | 18 | |
| Memory loss | 4 | 34 | 14 | |
| Sleep disturbance | 2 | 32 | 6 | |
| Rash/dermatitis | 7 | 31 | 18 | |
| Difficulty concentrating | <1 | 27 | NA | |
| Depression | 1 | 23 | NA | |
| Muscle pain | 1 | 21 | a | |
SOURCE: PAC, 1996.
NOTE: NA = Not available; values rounded to the nearest percent.
aIn the VA registry, muscle and joint pain combined are 17 percent.
Both the CCEP and VA Registry samples include only those persons who voluntarily sought a medical evaluation from these two clinical programs. Thus, these veterans may not be representative of the total population of troops deployed to the Persian Gulf region. In fact, according to the most recent DoD report on the CCEP (DoD, 1996), the following subgroups have been evaluated by the CCEP at a higher rate than their representation in the military population: female soldiers, African-Americans, those over 30 years of age and Army personnel. In addition, use of these data to measure the extent of health problems is limited by lack of information on the severity and chronicity of symptoms or illnesses reported (i.e., symptoms were measured at a point-in-time and information may not be available on how long symptoms persisted). Thus, the extent and magnitude of health problems experienced by veterans of the Gulf War can not be determined from CCEP and VA Registry data.
Several epidemiologic studies do suggest, however, that symptoms and self-reported chronic conditions occur at a higher rate in deployed personnel than in those who were not deployed. To estimate the scope of the likely impact of deployment, we briefly review below a few key epidemiologic studies (see the companion report by Sloss et al., 1998, for a more detailed review).
One study of Air National Guard personnel from four units found that the prevalence of each of 13 chronic symptoms of at least six months duration was much higher four years after Operation Desert Storm (ODS) in those deployed to the Gulf compared to those not deployed (Kizer et al., 1995; also see Centers for Disease Control, 1995; Fukuda et al., 1998). The excess was most pronounced for diarrhea (4-12 times higher in the deployed) and lowest for headache (1.3-1.6 times higher). Similarly, in a large epidemiologic study of Gulf War veterans and their non-Gulf War counterparts who listed Iowa as their home state, health problems were reported at a higher rate by deployed personnel (The Iowa Persian Gulf Study Group, 1997). Deployed regular military personnel reported greater levels of depression (16 percent versus 11 percent), post-traumatic stress disorder (1.9 percent versus 0.7 percent), chronic fatigue (1.0 percent versus 0.2 percent), cognitive dysfunction (17.7 percent versus 7.4 percent), bronchitis (3.2 percent versus 2.8 percent), asthma (6.7 percent versus 3.8 percent), fibromyalgia (18.2 percent versus 9.2 percent), alcohol abuse (17 percent versus 12.2 percent), anxiety (3.9 percent versus 1.9 percent) and sexual discomfort (1.2 percent versus 1.1 percent). Similar differences were found between deployed and nondeployed National Guard/Reserve personnel.
Bodily symptoms were also found to be related to deployment status in studies of active duty and Reserve personnel from the states of Pennsylvania and Hawaii two years post-ODS (Walter Reed Army Institute of Research, 1994; Stretch et al., 1995). For example, active duty deployed troops compared to nondeployed troops reported significantly higher symptom levels (in 20 out of 23 symptoms measured) including: headaches (45 percent versus 24 percent), back problems (29 percent versus 15 percent), allergies (13 percent versus 9 percent) stomach upset (22 percent versus 8 percent) muscle aches (27 percent versus 13 percent), and aching joints (31 percent versus 16 percent).
In contrast, studies of more serious health problems (and those that can be measured more objectively) have found similar rates of disease-specific mortality in Gulf War veterans and their nondeployed military counterparts (Kang and Bullman, 1996) and similar rates of birth defects in offspring born in military hospitals to deployed and nondeployed veterans (Cowan et al., 1997). Finally, Gulf War veterans had similar rates of postdeployment hospitalization for most conditions, although Gulf War veterans did have an increased risk of hospitalizations for neoplasms (mostly benign), diseases of the genitourinary system, diseases of the blood, and mental disorders, including adjustment reactions, and drug and alcohol dependence (Gray et al., 1996).
Although the magnitude of health problems is as yet unknown, the symptoms found among Gulf War veterans do not appear unique to the Gulf War experience. Numerous studies of primary care populations indicate high rates of bodily symptoms similar to those reported by CCEP and the VA Registry participants (Koch, 1975; Kroenke, 1989). Fatigue, dizziness, insomnia, and various pain syndromes are among the leading complaints in primary care (Koch, 1975).[3] The frequency of somatic symptoms as a presenting problem in primary care clinics across a wide variety of cultures was demonstrated in a recent study by the World Health Organization, which showed an overall rate of about 20 percent in 15 centers around the world (Gureje et al., 1997). Even in community samples, somatic symptoms are common, with lifetime prevalence rates of 37 percent for joint pain, 31 percent for back pain, 25 percent for headache and 24 percent for fatigue (Kroenke and Price 1993). These studies are not fully comparable to the CCEP program, however, since Gulf War veterans tend to be younger and more likely to be male than are patient and community samples.
It should also be noted that symptoms and illnesses seemingly similar to those found among Gulf War veterans have been reported by soldiers of other wars (e.g., Hyams, Wignall, and Roswell, 1996). For example, during the Civil War, DaCosta evaluated 300 soldiers, identifying a syndrome called irritable heart that was characterized by diarrhea, dizziness, shortness of breath, sleep disturbance, headache, palpitations and chest pain (DaCosta, 1871). Similar constellations of symptoms were classified as soldier's heart or effort syndrome in World War I, battle fatigue in World War II, and were possibly attributed to Agent Orange exposure in the Vietnam War (Hyams et al., 1996). A companion report in this series describes the kinds of symptoms and responses experienced by soldiers in prior wars (Marlowe, forthcoming).
This report does not address, in detail, the historical literature on the role of stressful wartime experiences on morbidity. A detailed discussion of this topic is provided in a companion report by Marlowe (forthcoming). That report describes the health consequences of participation in war and posits that observed differences are due, at least in part, to historical variation in cultural beliefs, differences in medical knowledge, and attributions about causation. In addition, Marlowe posits that predispositions and vulnerabilities, as well as cultural differences, help shape illness responses (i.e., subjective experiences of physical or emotional symptoms) in the context of deployment and combat. As suggested by Marlowe (forthcoming), it is likely that symptoms reported by Gulf War veterans are multifactorial in nature and not due to a single cause.
With regard to the general literature on stress, health, and related topics, we identified several thousand articles spanning several decades. To narrow our focus, we emphasized research published within the past 15 years that appeared in peer-reviewed scientific journals. In all, we consulted more than 250 articles, books, and technical reports, including both theoretical and empirical analyses. The review spanned a range of topics, including the nature of stress and the stress process, the role of stress and other risk factors in contributing to poor health, the pathways by which stress is linked to poor health, and the types of illnesses and diseases associated with stress. With respect to the literature concerning stressors faced by personnel deployed to the Persian Gulf, we identified approximately 55 pertinent research articles, book chapters, and technical reports. As noted in the chapter detailing this information, we focused on key surveys of Gulf War personnel administered both during deployment and after the war's end.
As for studies pertaining directly to the putative link between stress and health problems experienced by Gulf War veterans, we consulted approximately 60 articles and technical reports that presented original data as well as review articles and editorials.
[1]At the time of this report, actual data were available on roughly 70,000 veterans.
[2]The term "ill-defined" is used in the ICD-9 classification system and refers to symptoms for which a clear diagnosis could not be established. Some of these symptoms are consistent with those considered to be functional or somatoform symptoms.
[3]In a study of primary care active-duty military personnel and their dependents, as well as retired service members, 38 percent of the sample reported one or more symptoms (e.g., chest pain, fatigue, dizziness, headache, edema, back pain, dyspnea, insomnia, abdominal pain, numbness, impotence, weight loss, cough, constipation) during a three-year period (Kroenke and Mangelsdorff, 1989).