Military Medicine in Operations Desert Shield and
Desert Storm:
The Navy Forward Laboratory, Biological Warfare
Detection, and Preventive Medicine
Background
When U.S. troops were deployed to Saudi Arabia in August 1990, military medicine was
prepared for the unique health risks our troops faced in the Persian Gulf. The U.S.
military operates a network of six overseas infectious disease research laboratories,
which serve as training sites for military medical personnel and scientists (1). These
laboratories are regional centers of excellence for basic and applied research that
benefit both the U.S. military and host nations by identifying infectious disease risks
and developing improved prevention, control, and treatment measures.
One of the oldest overseas laboratories is located in Cairo, Egypt: the U.S. Naval Medical
Research Unit No. 3 (NAMRU-3). NAMRU-3 has operated continuously since 1946, including the
7-year period (1967 to 1973) when there was a break in diplomatic relations between the
USA and Egypt (2). NAMRU-3 has a long and distinguished record training U.S. and foreign
medical personnel, assisting local health ministries and the WHO, and representing the
United States abroad.
The research efforts at NAMRU-3 are extensive and include vaccine and drug development and
disease surveillance. Research investigations frequently involve field studies in various
countries in the Middle East, where numerous temporary laboratories have been established
over the last 40 years (2). Consequently, when Operation Desert Shield began, the Navy had
a sophisticated diagnostic laboratory and an active research and surveillance program in
the Middle East, plus medical personnel with extensive experience in this region. U.S.
Navy doctors and scientists knew what infectious diseases threatened our troops;
understood what diagnostic tests were needed in Saudi Arabia; and, most critically, knew
how to effectively operate in this region.
Navy Forward Laboratory
Beginning in August 1990, U.S. Navy preventive medicine personnel and scientists began
evaluating infectious disease risks among deployed troops. In September 1990, the Navy
Forward Laboratory (NFL) was established at the "Marine Corps Hospital" in
El-Jubail, Saudi Arabia (3). The "Marine Corps Hospital" was an unoccupied
civilian hospital that had all the requirements to accommodate a modern diagnostic
laboratory: an unused clinical facility, running water, and climate control. Laboratory
equipment and supplies were quickly flown into the theater by commercial airlines from
Cairo, Egypt, the U.S. Navy Environmental and Preventive Medicine Unit No. 7 (NEPMU-7) in
Naples, Italy, and various medical facilities in the USA.
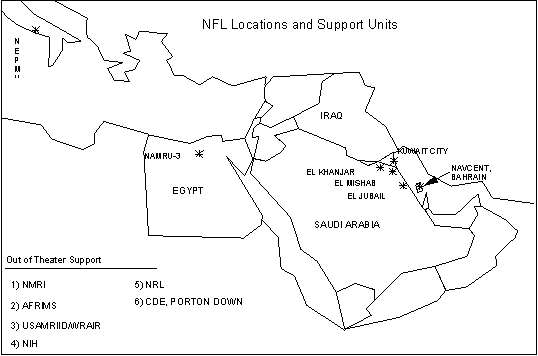
The Navy Forward Laboratory in El-Jubail, Saudi Arabia; satellite laboratories established
by the NFL in El Mishab, El Khanjar, and Kuwait City; and out of theater support for the
NFL during the Persian Gulf war.
The NFL eventually had a staff of eight personnel: four Medical Service Corps officers
(microbiologists), two Medical Corps officers (infectious diseases specialists), and two
Hospital Corpsmen (advanced laboratory technicians). The NFL was attached to the Naval
Logistics Support Command and reported directly to the NAVCENT Surgeon, whose leadership
was critical in establishing and maintaining the laboratory. The NFL developed into a
state-of-the-art infectious disease diagnostic laboratory that had the capabilities of a
well-equipped laboratory in the USA, including DNA probes and polymerase chain reaction
(PCR) analysis (3). When fully operational, the NFL served as the theater-wide, infectious
diseases reference laboratory for coalition forces.
Naturally Occurring Infections
During Operation Desert Shield, the main focus of the NFL was to analyze blood and stool
samples from patients and to assist preventive medicine personnel. In order to carry out
these duties, the staff of the laboratory maintained two rental cars, which were used
extensively to travel throughout Northeastern Saudi Arabia, evaluating patients and
assessing health risks.
During these travels, one of the first questions that arose pertained to the numerous
piles of dead animals that were scattered across the desert. Beginning in August 1990,
these collections of dead animals were evaluated by U.S. veterinary personnel, who
determined that their deaths were due to natural causes among the large herds of sheep,
goats, and camels kept by the Bedouin in this region (4). The local residents left the
dead animals in specific locations for counting and compensation from the government (5).
In the desert, these dead animals tended to dry out rather than rot quickly.
The piles of dead animals naturally were of concern to U.S. troops who camped near these
locations (4). Although the animals themselves were not thought to pose a direct health
risk, they were considered to be a potential breeding ground for insect-transmitted
diseases. As a result, military entomologists thoroughly sprayed the piles of dead animals
with insecticides. This spraying may explain some subsequent reports of dead animals and
insects, particularly among troops who arrived in Saudi Arabia in January and February
1991 at the start of the war. These newly arrived troops would not have known that dead
animals had been in the desert for at least five months before hostilities began.
Acute diarrheal disease and common-colds were the main infectious disease problems during
the early stages of the deployment. Epidemiological surveys indicated that approximately
two-thirds of ground troops had acute diarrhea during both Operation Desert Shield and
Desert Storm (6). Nearly all cases of diarrhea were due to the infectious agents NFL
personnel had identified during prior deployments of U.S. troops to the Middle East,
mainly traveler's type diarrhea ("tourista" or the "trots") and Shigella.
No case of typhoid fever, cholera, or amoebic dysentery was identified by laboratory
analysis (6).
U.S. troops also frequently had acute upper respiratory infections and complaints (cough,
sore throat, sneezing, runny nose), which occurs any time troops are crowded together and
rapidly deployed overseas. There also was concern that the fine blowing sand in Saudi
Arabia was causing respiratory problems. However, epidemiological surveys determined that
respiratory symptoms were more common among the minority of troops who worked and slept in
air-conditioned buildings than among personnel living in tents or open warehouses (7).
Troops living in tightly constructed buildings had more symptoms because in closed and
crowded spaces they were more likely to pass respiratory infections among each other.
These respiratory infections were found on analysis in the NFL to be caused by common
viral and bacterial agents, like influenza (6).
A major concern for medical personnel was the threat of two infectious diseases (sand fly
fever and leishmaniasis) that are transmitted by sand flies, because they had caused
problems for U.S. and British troops during World War II. Extensive surveillance and
testing of U.S. troops, however, did not identify a single case of sand fly fever, and
only 12 cases of visceral and 20 cases of cutaneous leishmaniasis were diagnosed after the
war among over 750,000 U.S., British, and Canadian Gulf war veterans (8). In addition, the
sand fly vectors could not be found during and after the war in most locations where our
troops were deployed (6, 9). The very low number of illnesses caused by sand flies and
other insects may have been due to:
1) the deployment of most troops to barren desert locations where sand flies and their
animal hosts do not live;
2) the deployment of most U.S. troops during the cooler winter months of December to
February when insects are least active; and,
3) the use of insecticides and repellents.
There were only seven cases of malaria, three cases of Q-fever, one case of West Nile
fever, and no case of brucellosis identified among U.S. troops (6). The infectious
diseases diagnosed during this wartime deployment were the same ones found in peacetime
when U.S. troops are sent to the Middle East. Although preventive measures can reduce the
risk of diarrheal and respiratory infections, these common infections cannot be totally
avoided during crowded deployments to tropical and developing countries. The only
possibility for complete prevention is from research and development of effective vaccines
and preventive measures.
Biological Warfare Detection Capabilities
During Operation Desert Storm, the emphasis of the NFL shifted from routine infectious
disease problems to the threat of biological warfare (BW) (3). From the beginning of the
deployment, it was clear that to protect U.S. and coalition troops against the potential
use of biological warfare, an in-theater laboratory capable of detecting BW agents was
essential. Therefore, the NFL diagnostic capabilities and staff were augmented during
Operation Desert Shield to deal with the threat of biological warfare. At the start of
Operation Desert Storm, the NFL was prepared to detect potential BW agents.
The techniques used for the identification of potential BW agents were developed by
worldwide experts and represented existing state-of-the-art test methods. The NFL used
technologies that encompassed a full range of laboratory techniques, including:
1) bacteriological identification and microscopy;
2) immunologic-based assays for detecting bacterial and viral antigens and antibodies;
and,
3) molecular techniques, like PCR.
Various types of samples could be analyzed in the NFL, both biological samples (like
blood) and environmental samples from soil, water, and air collectors.
The most likely BW threat from Iraq, based on the best intelligence at the time, was from
the use of weapons loaded either with the bacterium, Bacillus anthracis, or
with the botulinum toxin -- a toxin produced by the bacterium, Clostridium botulinum.
The bacteria that cause anthrax and botulism both occur naturally in the environment.
Anthrax affects livestock and causes disease among humans working closely with infected
animals or their hides. Anthrax is a good BW agent because when inhaled, it causes rapid
death from massive bleeding in the lungs. Botulinum toxin is a highly lethal substance,
which causes disease in the United States when contaminated food is improperly canned or
stored. Because this toxin causes very rapid paralysis and death in minute amounts, it is
ideal for biological weapons production.
The extensive number of assays maintained in the NFL were capable of detecting not only
the most likely BW agents (anthrax and botulinum toxin) but also additional, potential
bacterial, viral, and toxic agents. Samples received and analyzed at the laboratory also
were sent to laboratories in the United States (U.S. Army Medical Research Institute of
Infectious Diseases, Ft Detrick, MD) and the United Kingdom (Chemical Biologic Defense
Establishment, Porton Down) for further confirmatory analysis.
As previously noted, a common observation in the theater of operation was the piles of
dead animals. During the course of the war, samples from seven dead goats were analyzed by
the Navy Forward Laboratory BW team. Using the array of laboratory techniques available in
the NFL, no BW agent was detected in these samples. Also, 33 samples from air collectors
stationed around the theater of operation did not contain evidence of BW contamination.
Other samples analyzed by the NFL and found negative for BW agents included water samples
obtained after the war from the Royal Palace in Kuwait City.
Because of the inherent limitations of any laboratory test, especially newly developed
assays, all samples analyzed for BW agents were subjected to repeated testing with
dissimilar assay methods to confirm results. Multiple tests are required when the results
involve an important question, such as potential exposure to BW or CW agents, because no
test for biological or chemical agents is foolproof. Even in the routine hospital and
outpatient clinic setting, multiple tests are often required to diagnose a patient's
condition because of the limitations of any test method.
Although requiring additional time and labor, this concept of overlapping and different
assay methods had the benefit of significantly enhancing the range and accuracy of the BW
detection capability in the NFL during the Persian Gulf war. For example, infectious or
chemical agents contained in a sample may be in such a form or amount that it cannot be
detected by one method alone. In addition, there is the problem of false negative and
false positive test results, which are unavoidable problems with all assays. By using
different tests to analyze samples, questionable test results could be identified and
corrected.
Despite a search for BW agents from clinical, environmental, and veterinary samples, no
evidence of a BW agent was detected during Operation Desert Shield or Desert Storm.
Nevertheless, one of the lessons learned during the Gulf war was the necessity to have an
in-theater biological laboratory, like the NFL, when large numbers of troops are deployed.
Identification of biological agents in-theater provides an early warning capability of
hostile BW usage, allowing for timely implementation of effective prophylactic and
therapeutic measures.
Another lesson learned was that more rapid BW assay methods are needed, which has been the
focus of the military's biological defense research program since the Persian Gulf war.
The present number of BW agents that can be detected is now much expanded. New methods
also have been designed to detect BW agents in a broad range of substances other than
clinical samples, including soil and sand samples, water samples, and even samples
obtained from hard surfaces by swabbing. A greatly improved version of a rapid assay for
BW agents has been developed at the U.S. Navy Medical Research Institute (NMRI), Bethesda,
MD. Assays similar to standard pregnancy tests are capable of detecting a growing list of
BW agents in about 15 minutes.
Summary
The NFL provided a critical diagnostic capability during Operations Desert Shield and
Desert Storm that added to DoD's effective patient care and preventive medicine efforts.
Just as importantly, the NFL provided commanders with accurate information about the
nature of the biological threat during this wartime deployment.
There were two principal reasons for the success of the NFL. For one, the military's
network of overseas infectious diseases research laboratories was essential. These
laboratories offer specialized training for DoD personnel in foreign environments and
provide support during deployments. The other reason for the success of the NFL was the
early recognition and acceptance of the laboratory by all echelons of command,
particularly the support provided by BUMED 02 and the NAVCENT Surgeon.
Since the end of the Gulf War, the forward laboratory concept has been institutionalized
into the Forward Deployed Laboratory (FDL), under the coordination of the Navy
Environmental Health Center (NEHC), Norfolk, Virginia. When deployed, this laboratory is
composed of a "core" infectious disease diagnostic capability. Layered on top of
this "core" are specialized capabilities (modules), such as BW detection.
Presently, the BW detection module is provided by the Biological Defense Research Program
(BDRP) at the Naval Medical Research Institute (NMRI), where a mobile laboratory for BW
detection has been developed.
The NMRI mobile BW laboratory additionally has critical national security uses outside of
military deployments. NMRI laboratory personnel and the mobile laboratory have been
utilized to actively support U.S. and international agencies in countering BW threats,
including the United Nations controlled sanctions of Iraq and the recent question of a
biological threat in a package left at B'nai B'rith in Washington, DC.
Preventive Medicine and Surveillance
During Operations Desert Shield and Storm, the U.S. military initiated extensive disease
prevention, control, and surveillance efforts (6,10). The Preventive Medicine (PM)
activities among U.S. Marine Corps troops provided one example of this comprehensive
effort. When U.S. Marines deployed to the Persian Gulf in August 1990, PM personnel were
among the first to arrive. Because of the medical threats that Marine Corps units face
during deployments, highly trained PM specialists are "built into" the Marine
Table of Organization at multiple levels. Preventive medicine experts are assigned to
front line units of the Division and Wing, to the combat medical support elements of the
Force Service Support Group, and to the highest headquarters levels. These specialists
know what illnesses might affect Marines and sailors in a particular area, like the
Persian Gulf, and how to prevent health problems in field settings.
Within the First Marine Division, an Environmental Health Officer (EHO) is assigned to the
Division Surgeon's staff to advise on key PM issues, such as field sanitation, protection
of food and water, proper immunizations, and the prevention of insect-borne diseases. At
the unit level, a PM Technician (PMT) works within the battalion medical department to
carry out basic PM measures. The PMT's and the EHO's worked together during the Persian
Gulf deployment to insure that:
1) food and water were safe to consume;
2) field sanitation measures were in place to prevent the
spread of disease;
3) flies and other insects were controlled; and,
4) proper immunizations were received.
Preventive Medicine personnel also advised unit leaders on the prevention of heat
casualties and on the appropriate countermeasures for biting insects. The Marine Aircraft
Wing has its own EHO assigned to the Wing Surgeon's staff, and PMT's at each Marine
Aircraft Group perform similar functions. Naval Mobile Construction Battalions (SeaBee's)
assigned to Marine forces also had a similar PM capability built into their structure.
From the beginning of Operation Desert Shield, PM personnel were serving at the front
lines, using their knowledge and experience to identify and prevent potential health
problems before they affected the Marines' vital mission.
At the Medical Battalion of the First Force Service Support Group (FSSG), a large PM
section was deployed, which consisted of EHO's, entomologists (experts in insect and pest
control) and a team of PMT's, augmented with additional personnel from a Navy Disease
Vector Ecology and Control Center, Jacksonville, Florida. This section brought extensive
PM equipment and supplies, including insect and rodent control products, water testing
gear, and chlorine to purify water. Their mission was to provide higher level back-up for
the first line PM personnel at Division and Wing. This enhanced capability was positioned
with Combat Service Support Detachments in support of forward Wing and Division units. In
addition, the Medical battalion PM section provided direct support to battalions in the
FSSG. Together, the Marine Corps PM teams ensured the very best in field preventive
measures, where and when they were needed most.
Surveillance
One of the most important priorities in any PM effort is to recognize disease and
non-battle injury (DNBI) problems early, while they can be more readily controlled. For
the first time in U.S. Marine Corps history, a system of DNBI surveillance was established
at the beginning of the Gulf deployment to track key illness and injury rates at virtually
every Marine and SeaBee Medical Aid Station. A Navy Preventive Medicine physician was
augmented to the MARCENT Surgeon's staff at the beginning of the operation to continuously
analyze DNBI rates and identify any unusual patterns. In addition, all admissions to
medical battalion facilities or Navy Fleet Hospitals were continuously monitored
throughout the Gulf deployment to detect unusual or unanticipated diseases.
By tracking actual DNBI rates and trends in nearly all units, PM personnel were in
position to respond immediately to problems and apply appropriate countermeasures. Based
on the expected medical threats in the Persian Gulf, special attention was focused on the
following DNBI categories, which were devised specifically to identify health problems
that could degrade combat effectiveness:
Heat injury -- one of the most significant health threats early in the deployment;
Diarrhea -- a potentially epidemic problem in field conditions;
Skin conditions -- a significant cause of lost man-days in many previous conflicts;
Respiratory conditions -- colds, pneumonia and other respiratory problems are
common and can be widespread during any deployment;
Injury/musculoskeletal conditions -- a major cause of lost man-days from training
and
deployment activities;
Eye problems -- eye infections, such as "pink eye," can be epidemic in
field conditions,
and corneal abrasions from blowing sand was also a risk in the desert;
Unexplained fevers -- an unexplained fever may be the first sign of diseases, such
as sand fly fever, malaria, and other serious infections;
Psychiatric conditions -- the stresses of deployment and combat often manifest in
psychiatric symptoms;
Other conditions -- other problems seen at sick call not fitting into the above
categories.
Each week, unit aid stations reviewed their sick call logbooks and determined how many
Marines or sailors were treated for the above categories of health problems. A
unit-specific DNBI rate was then calculated for each category, based on how many Marines
or sailors were assigned to the unit. These simple calculations allowed PM personnel to
determine what percentage of the unit was treated during the prior week for these key
problems. If the percentage was higher than expected, the cause was investigated.
The DNBI surveillance system demonstrated that PM efforts were very successful in keeping
Marines and sailors healthy during Operations Desert Shield and Desert Storm. On average,
approximately six percent of ground troops were treated per week for some type of illness
or injury. This compares favorably to the DNBI rates in garrison troops at Camp Pendleton,
California, where approximately four percent of personnel per week are treated.
Furthermore, DNBI rates decreased during the deployment as troops adapted to field
conditions and PM efforts identified and controlled health threats.
Total weekly rates of outpatient visits among approximately 40,000 Marine Corps ground
troops stationed in northeastern Saudi Arabia.
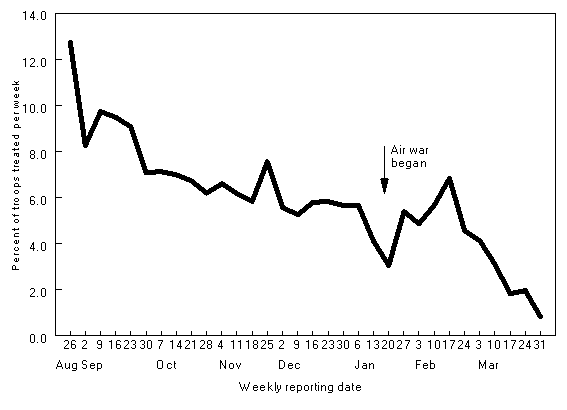
DNBI surveillance proved its worth early in the deployment, when elevated diarrhea rates
were detected simultaneously in numerous U.S. Marine units located throughout Saudi
Arabia. The force-wide average diarrhea rate rose to approximately four percent per week,
with some units experiencing significantly higher rates. Recognizing these elevated
diarrheal rates early enabled PM personnel to rapidly identify specific problems with the
contract food sources that had to be used in the initial stages of a rapid wartime
deployment. Fresh produce initially procured outside of the normal supply system was shown
by the Navy Forward Laboratory to contain local, diarrhea causing bacteria (6). This
problem was rapidly corrected, and diarrhea rates quickly dropped below one percent per
week for the remainder of the deployment. This rate of illness is only slightly higher
than the normal diarrhea rate seen in garrison at Camp Pendleton.
Weekly rates of gastroenteritis among outpatients in approximately 40,000 Marine Corps
ground troops stationed northeastern Saudi Arabia.
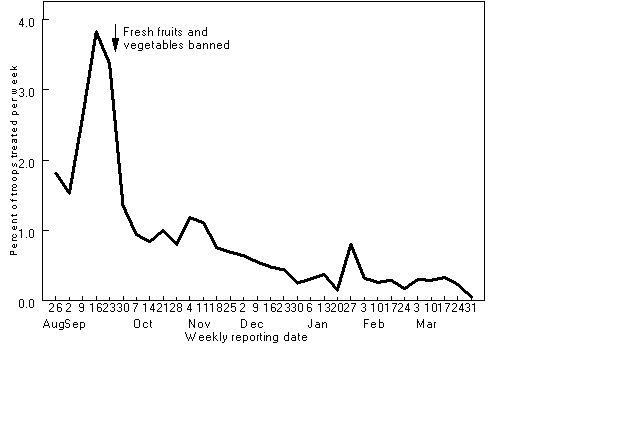
Respiratory disease rates remained generally low during Operations Desert Shield and
Storm, with few cases requiring hospitalization. Rates of outpatient treatment were
slightly higher early in the deployment when troops tended to be crowded together during
air travel and in staging areas. Respiratory disease rates rapidly declined as troops
spread out, but rose again when the weather turned cold. These acute respiratory illness
patterns are similar to what is typically seen in the U.S. and were not a significant
problem for U.S. Marines. The British also experienced increased rates of respiratory
disease during periods of deployment and crowding (6). It is noteworthy that treatment for
respiratory complaints did not increase from exposure to smoke after the Iraqi army
ignited over 600 oil well fires in Kuwait a the end of the war.
Weekly rates of respiratory disease among outpatients in approximately 40,000 Marine Corps
ground troops stationed in northeastern Saudi Arabia. The arrows indicate the two primary
periods of time when U.S. Marine Expeditionary Force (MEF) personnel were being deployed.
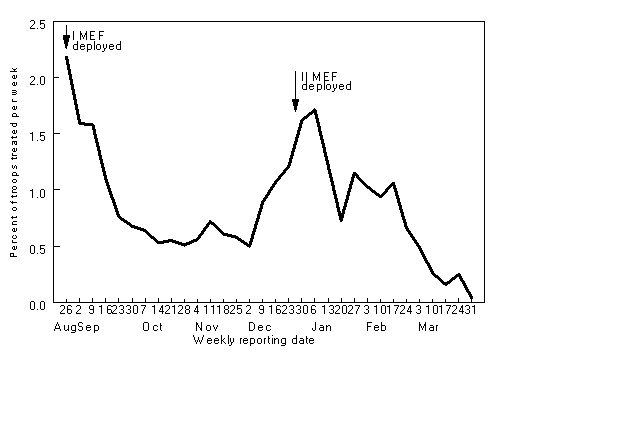
In all other DNBI categories, illness rates were remarkably low. In spite of extremely hot
and humid conditions at the beginning of the deployment, less than 0.3% of the force per
week (3 cases per 1000 per week) required treatment at an aid station for heat injury.
Strong Command emphasis on providing abundant water and acclimatizing troops scored a
major victory against this major health threat. In addition to these low rates, only about
one percent of the force was treated per week for skin problems, mainly fungal infections
and heat rash. This rate is comparable to that seen in garrison setting during hot and
humid conditions.
Importantly, the surveillance system did not detect either sand fly fever or cutaneous
leishmaniasis (which causes skin sores) among U.S. Marines. These infectious diseases are
transmitted by sand flies and were expected to be major problems in the Persian Gulf.
Entomologist, PMT's and EHO's were on constant lookout for sand fly vectors, but very few
were identified.
All other DNBI rates, including injuries, eye problems, psychiatric conditions, and
unexplained fevers were remarkably low throughout the deployment, and well within the
expected norms. It is noteworthy that the rate of unexplained fevers remained essentially
zero throughout the deployment. This DNBI category was designed as an early warning
indicator to detect unusual insect-borne infections, such as sand fly fever, malaria, and
dengue. Most of these infections take time to diagnose, but they typically begin with an
acute febrile illness. The absence of unexplained fevers was reassuring to medical and PM
personnel, indicating that Marines and sailors were not experiencing serious infections.
This finding was corroborated by the near absence of disease carrying sand flies and
mosquitoes during the deployment. Furthermore, no individual was hospitalized for these
illnesses during the deployment, except for one case of West Nile fever -- an acute
flu-like viral infection (6).
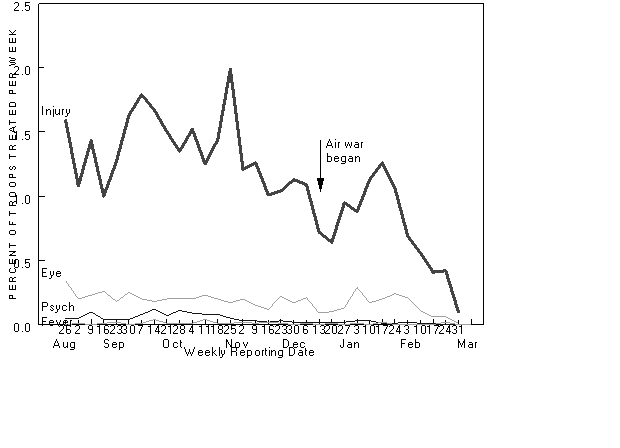
Weekly rates of outpatient visits for injuries, eye problems, psychiatric evaluation, and
febrile illness among approximately 40,000 Marine Corps ground troops stationed in
northeastern Saudi Arabia.
Although this pioneering system of DNBI surveillance was not perfect, it was a critical
tool in immediately defining the major patterns of illness and injury in each Marine unit
for most of the deployment. Combined with hospital surveillance, it clearly demonstrated
that U.S. Marine Corps and Navy ground personnel remained very healthy during Operations
Desert Shield and Storm. Also, when a problem arose, it was quickly identified and
overcome.
This DNBI surveillance system proved so successful that it was adopted as the standard
approach for all subsequent joint deployments involving U.S. military personnel. It has
been modified and successfully used during Operation Restore Hope in Somalia, during the
Haiti intervention, and during the current operation in Bosnia.
Conclusion
The U.S. military was ready for the health threats our troops encountered in the Persian
Gulf war. As a result, the disease non-battle injury (DNBI) rate during this war was lower
than in previous major conflicts involving U.S. military personnel (11,12). The good
health of U.S. troops was due in part to comprehensive preventive medicine efforts,
accurate and rapid laboratory diagnosis, and the extensive health care system that was
established in Saudi Arabia during Operation Desert Shield (13).
Besides these medical measures, several fortunate circumstances aided U.S. troops,
including:
1) deployment to barren desert locations during cooler
winter months when insect activity is lowest;
2) limited contact with non-military populations;
3) very limited access to alcohol; and,
4) the great strides made in Saudi Arabia and Kuwait during
the last several decades in public health and the elimination of
local diseases.
Although wars cannot be conducted as large epidemiological studies, greater infectious
disease diagnostic and surveillance information was collected on U.S. troops during the
Persian Gulf deployment than in prior wars. Since the end of the Persian Gulf war, these
data have aided investigators in the search for the causes of veterans' health problems.
To date, the primary chronic infectious disease problem identified among veterans has been
12 cases of visceral leishmania infection. Nevertheless, investigations are continuing for
other possible chronic infectious disease problems.
The principal unanswered health question following the war with Iraq has been the unknown
nature and causes of the unexplained symptoms experienced by some Gulf war veterans.
Because similar physical symptoms have been reported by war veterans since the U.S. Civil
War (14), hard to answer questions about veterans' health could arise after future wars.
The improved surveillance and diagnostic methods pioneered during the Persian Gulf war and
more recent improvements in medical record keeping will help the DoD and VA provide the
best health care possible for both current and future veterans.
Bibliography
1. Gambel JM, Hibbs RG. U.S. Military overseas research laboratories. Mil Med
1996;161:638- 645.
2. Hibbs RG. NAMRU-3: forty-six years of infectious disease research. Mil Med
1993;158:484-488.
3. Hyams KC, Bourgeois AL, Escamilla J, Burans J, Woody JN. The Navy Forward Laboratory
during Operations Desert Shield/Desert Storm. Mil Med 1993;158:729-732.
4. Spencer L. Colonel Alm recounts vital role of veterinarians in Persian Gulf
conflict. J Am Vet Med Assoc 1991;199:305-309.
5. Persian Gulf Veterans Coordinating Board. Unexplained iillnesses among Desert Storm
veterans: a search for causes, treatment, and cooperation. Arch Intern Med.
1995;155:262-268.
6. Hyams KC, Hanson K, Wignall FS, Escamilla J, Oldfield EC. The impact of infectious
diseases on the health of U.S. troops deployed to the Persian Gulf during Operations
Desert Shield and Desert Storm. Clin Infect Dis 1995;20:1497-1504.
7. Richards AL, Hyams KC, Watts DM, Rozmajzl PJ, Woody JN, Merrell BR. Respiratory
disease among military personnel in Saudi Arabia during Operation Desert Shield. Am J
Public Health 1993;83:1326-1329.
8. Magill AJ, Grogl M, Gasser RA, Sun W, Oster CN. Visceral infection caused by
Leishmania tropica in veterans of Operation Desert Storm. N Engl J Med 1993;328:1383-1387.
9. Cope SE, Schultz GW, Richards AL, et al. Assessment of arthropod vectors of
infectious diseases in areas of U.S. troop deployment in the Persian Gulf. Am J Trop Med
Hyg 1996;54:49-53.
10. Wasserman GM, Martin BL, Hyams KC, Merrill BR, Oaks HG, McAdoo HA. A survey of
outpatient visits in a United States Army Forward Unit during Operation Desert Shield. Mil
Med 1997;162:374-379.
11. Lindsay GC, Dasey C. Operations Desert Shield/Storm infectious disease rates: A
fortuitous anomaly. United States Army Medical Research and Development Command News
1992;February:5-6.
12. Defense Science Board. Report of the Defense Science Board Task Force on Persian
Gulf War Health Effects. Washington, DC: Office of the Under Secretary of Defense for
Acquisition and Technology; June 1994.
13. Blanck RR, Bell WH. Special reports: Medical aspects of the Persian Gulf war.
Medical support for American troops in the Persian Gulf. N Engl J Med 1991;324:857-859.
14. Hyams KC, Wignall FS, Roswell R. War syndromes and their evaluation: From the U.S.
Civil War to the Persian Gulf War. Ann Intern Med 1996;125:398-405.
For additional technical information please click on the following
articles:
The Navy Forward Laboratory during Operations Desert Shield/Desert Storm. Mil Med
1993;158:729-732.
The impact of infectious diseases on the health of U.S. troops deployed to the Persian
Gulf during Operations Desert Shield and Desert Storm. Clin Infect Dis 1995;20:1497-1504.
War syndromes and their evaluation: From the U.S. Civil War to the Persian Gulf War.
Ann Intern Med 1996;125:398-405.
-end-
Return to Medical Information
| First Page | Prev Page | Next Page | Back to Text |




